Now that spring is upon us, bats have started to emerge from hibernation or migrate back north, and some people are bound to encounter them. Many people are afraid of bats, some due to their link to superstitions and intrinsic elusive nature, others due to their association with diseases, or maybe due to other misunderstandings. Although they are an important vector of the rabies virus, the stigmatization of their presence in urban environments and the threat they pose to humans and other animals is unfortunately exaggerated and unproportional to how much they end up suffering due to their proximity to us. Knowledge is a key factor in understanding that these animals are important and deserve dignity like any other animal, so we believe any “bad feelings” are most likely rooted in a lack of access to clear information that could settle any misconceptions people may have regarding the safety of humans and animals when coexisting with bats.
In 2025, the Western/Northern node of the Canadian Wildlife Health Cooperative (CWHC) noticed an increased number of bats sent for diagnostic assessment compared to previous years. The ultimate causes of death for a lot of these bats were associated with predation and human encounters leading to traumatic injuries. This follows past years’ trends on major causes of death or injury in bats, meaning that whatever the reasons for these trends are, they are an ongoing problem. All received bats went through a rabies risk assessment and 20% tested positive for rabies, but it is important to remember that this percentage does not represent the actual prevalence of rabies in free-ranging bat populations, since we only receive sick or dead animals and not healthy ones, which skews our data. Approximately 1% of wild bats in Canada may be infected with the virus, although this is not well studied and highly dependent on species.
This article aims to answer some of the questions people ask us about why they are important, common causes of death in bats, what diseases affect bats, bat encounters, and how rabies risks are investigated and managed. Enjoy!
Why are bats important?

Bats and our pets
A common reason for bats being found in and around households is due to our own pets’ curiosity. Dogs and (mainly) cats may find bats moving about and ultimately prey on them. This can be either primary (pets being talented hunters and capturing healthy bats), or secondary (pets finding sick bats and taking advantage of their vulnerability to play with or prey on them). Free-roaming cats are of special concern, as they are a significant predator of bats and can contribute to the rabies cycle.
Predation is suspected or confirmed during a post-mortem examination when tears, fractures, and puncture wounds compatible with bites are observed. Sometimes, the bat’s history makes diagnosis more straightforward, such as when an owner witnesses a pet interacting with the bat. If this is suspected, an assessment by the family veterinarian is warranted, including the updating of vaccinations, and the provincial rabies risk assessment veterinarian must be notified.
This topic may be sensitive to some owners. It is sometimes hard to picture our cute and lovely pets as potential predators, but understanding this risk is the first step to a safer lifestyle for your pet by limiting or completely eliminating contact with wildlife and unrestricted access to the outdoors, which decreases the risks of accidents and disease.
Pseudogymnoascus destructans and white-nose syndrome
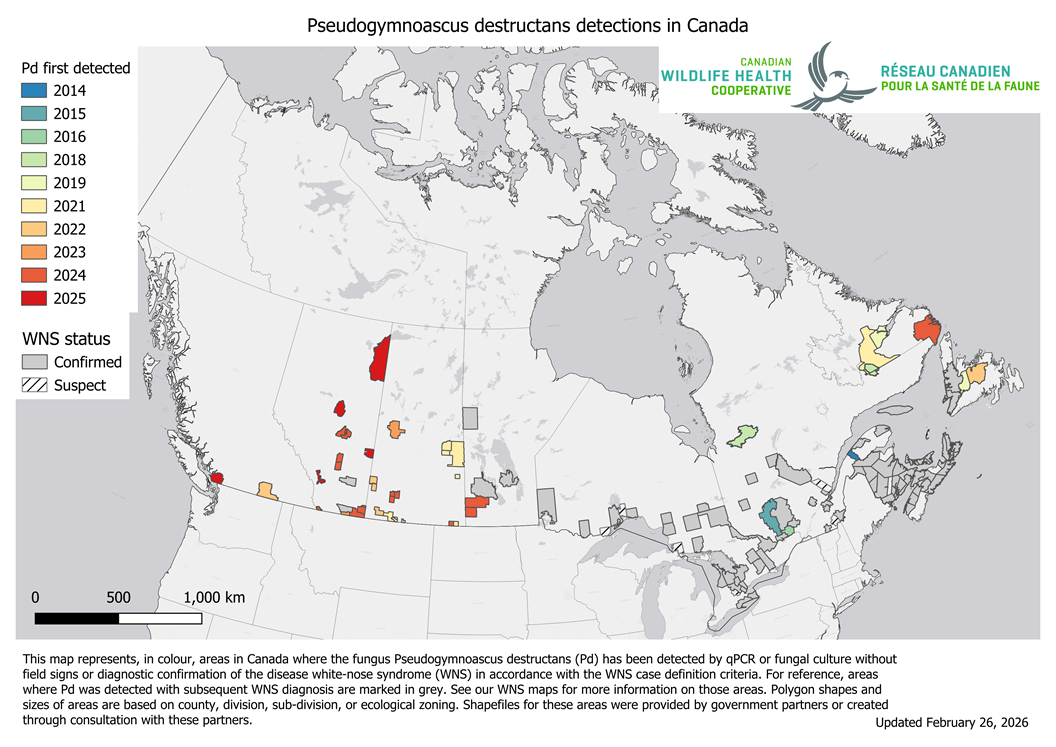
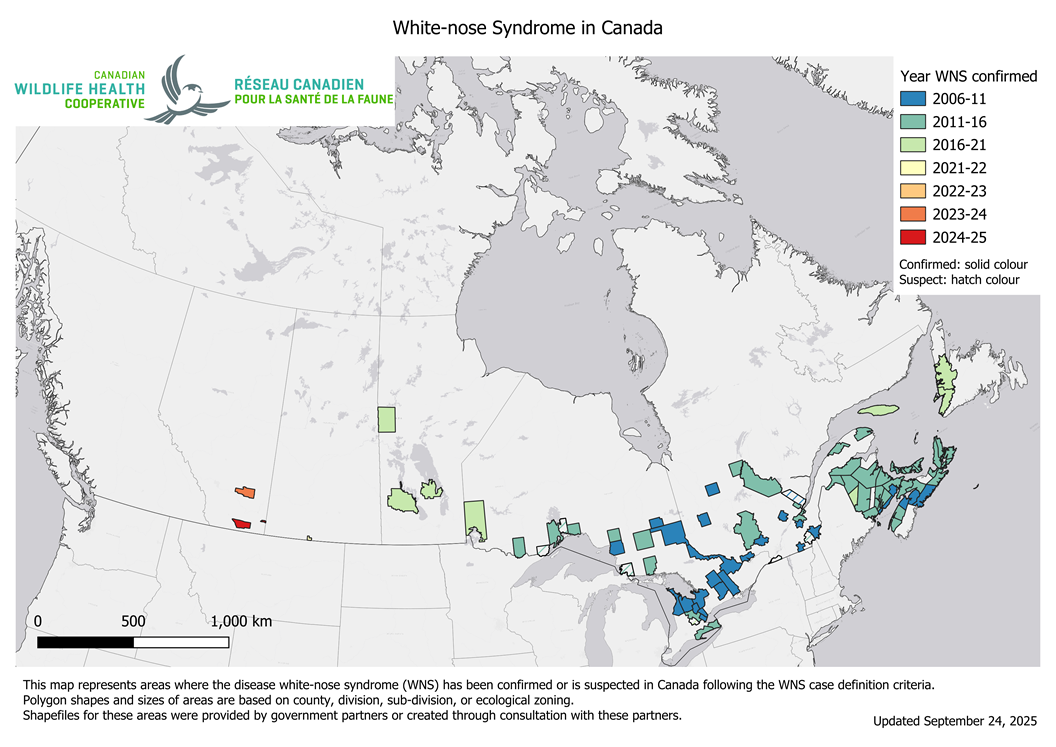
Pseudogymnoascus destructans, often abbreviated to Pd, is a cold-loving fungus that causes white-nose syndrome, a fatal disease that has decimated bat populations in North America. Many bat species live and hibernate in caves, the temperatures of which are in the range necessary for Pd to thrive. The fungus spreads onto the bats’ skin and disrupts their normal hibernation cycle, causing them to wake up too early. This depletes their fat reserves and leads the bats to die of emaciation.
The fungus was first found in Saskatchewan in 2021 (Map 1) and the Western/Northern region of the CWHC diagnosed white-nose syndrome in a little brown bat from Grasslands National Park in 2022 (Map 2). We have not diagnosed the disease in Saskatchewan since. However, just because we have not diagnosed white-nose syndrome since 2022 does not mean that bats are not dying of it. Most of our bat submissions come from Saskatoon and other urban areas where Pd has not been detected, and most of our bat submissions are big brown bats, which are relatively resistant to the disease. Additionally, big brown bats often live in man-made buildings and structures, places where Pd is not likely to establish.
Bats also suffer from rabies
Some people might imagine bats acting as carriers that are unaffected by rabies. This is not true. Although some bats can survive infection thanks to a generally resilient immune system, rabies is fatal once a bat develops clinical symptoms. Although not well studied and highly dependent on species, it is thought approximately 1% of wild bats in Canada may be infected with the virus.
The virus is spread through the saliva of an infected bat (or other animal), most commonly through bites, though saliva can also enter the body through a scratch, broken skin, the mucous membranes, or the respiratory tract. The virus then travels through the peripheral nervous system to the brain. In bats, this incubation period (the period between initial exposure and onset of symptoms) is highly variable and can range from several days to months or longer, though within 30 days is most common. Since the virus needs to travel to the central nervous system, the incubation time is proportional to the distance from the point of entry to the brain.
Bats who have contracted rabies often behave abnormally, though some appear normal or only show subtle signs of illness. Therefore, it is impossible to determine whether a bat has rabies just by observing it. Some signs that a bat could have rabies are:
- Active during the day
- Unable to fly
- Crawling on the ground
- Unusual “friendliness” or aggression
- Paralysis
- Being very vocal
Infected animals die within 10 days of becoming sick.
If you encounter a bat that is behaving abnormally, it is important not to handle it. Contact your local conservation officer or the Ministry of Environment Inquiry Centre for assistance. Your local wildlife rehabilitation centre may also be able to help with handling the bat and transporting it for testing.
Bat encounters
If you find a live bat in your house, garage, or other building, don’t panic. In most cases, direct contact can be avoided. However, if you have been bitten, scratched, or woke up to a bat (live or dead) in your bedroom, you should see your family doctor or local emergency room department as soon as possible to discuss rabies risk and next steps.
If a live bat has flown into a building and has not made direct contact with anyone, close the interior doors to prevent the bat from flying further inside. Open any windows and doors that lead outside and turn off any lights and ceiling fans. The bat can usually find its way back outside. If the bat has made direct contact with a person or animal and it is safe to do so, contain it so it can be tested for rabies.
If the bat does not leave on its own, it can be safely captured and released in the spring, summer, and fall months using a container with air holes and a piece of cardboard. Do not release bats outside in the winter as they will likely die; contact a licensed wildlife rehabilitator to overwinter the bat.
Make sure the container has airholes and close it securely so the bat can’t escape. Put the covered container with the bat somewhere quiet until nightfall, then take it outdoors to release it. Many bats cannot take flight from the ground, and you may need to elevate the container without the lid and tilt it so the bat can fly out. If the bat seems unable to fly, contact your local wildlife rehabilitator or the Ministry of Environment Inquiry Centre.
Bats are rarely aggressive but may bite when frightened, like all wild animals. Hence, it is our responsibility to interact with a wild animal in the safest way possible. Always wear thick gloves if potentially capturing bats, even if you are just trying to move them to a container – not because you should be “paranoid” about the animal, but because it is a great way to avoid an “unknown exposure” situation, where you are not sure if a bite or scratch could have happened without you noticing.
If you have found a dead bat outside or in your home, you can bring it to the Canadian Wildlife Health Cooperative lab in Saskatoon for testing or drop it off at a Ministry of Environment Field Office. Never handle dead wildlife without gloves or another barrier (e.g. inverted garbage bag) and always wash your hands afterwards.
Rabies testing
The diagram in Figure 2 explains the process of how rabies testing is performed in bats in Saskatchewan step-by-step.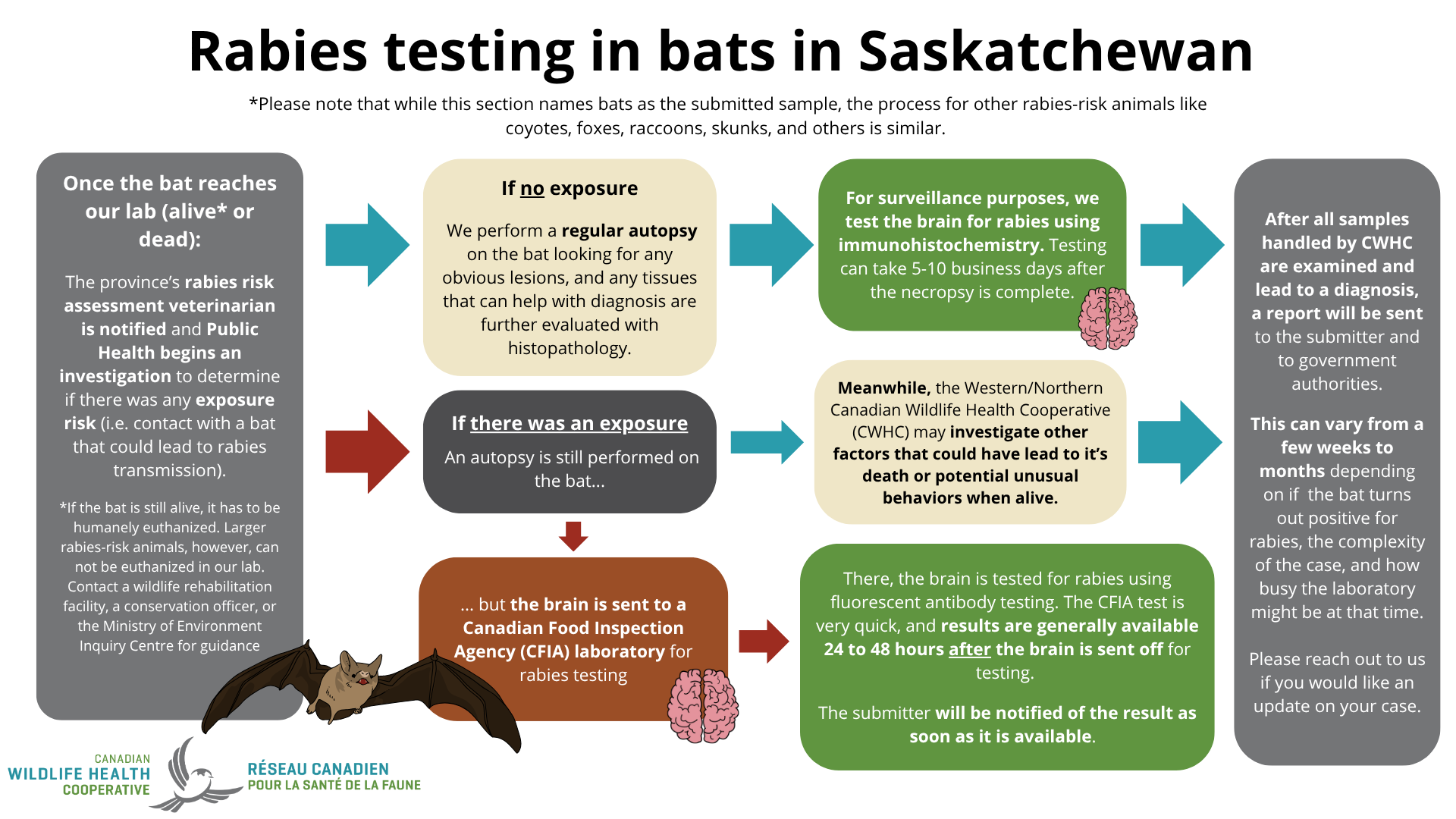
If the exposure did not occur recently, precautionary post-exposure prophylaxis may be recommended before testing is complete. If the test result is negative, no post-exposure prophylaxis is necessary. If the bat tests positive, post-exposure prophylaxis is pursued.
There is no charge for testing.
Post-exposure prophylaxis for humans
The rabies vaccine is not a routine immunization. Workers with high risk of occupational exposure to potentially rabid animals or the rabies virus should be immunized prior to the commencement of high-risk work. Travelers visiting high risk areas should receive pre-travel rabies immunization.
Post-exposure prophylaxis for immunocompetent people who have not previously been vaccinated against rabies consists of local wound treatment, rabies immunoglobulin given on day 0 (the day of health centre visit), and four doses of rabies vaccine given on days 0, 3, 7, and 14. People who are immunocompromised or are taking antimalarial drugs will receive a fifth dose of vaccine on day 28 and the level of neutralizing antibodies in the blood should be checked 7-14 days post-completion of the series to ensure an acceptable antibody response has developed.
Post-exposure prophylaxis for people who have previously been appropriately vaccinated against rabies consists of local wound treatment and two doses of rabies vaccine given on days 0 and 3. Rabies immunoglobulin is not necessary if a recent titer check indicated sufficient immune response.
Appointments will be scheduled to receive the vaccine after the initial immunization on day 0, which will take place at a Saskatchewan Public Health office during the week or a medical clinic if any of the vaccination days fall on a weekend.
Rabies prophylaxis for domestic animals
Rabies is best prevented by vaccinating your pets before exposure occurs, even if they are an indoor-only pet. Dogs and cats as young as three months old can be vaccinated against rabies, with a booster shot being required one year later. It takes 28 days for an adequate level of protection to be established after the first vaccination, so owners should be aware that puppies and kittens are not immediately protected after the first dose. Subsequent booster shots are required every one to three years depending on the vaccination schedule used, and the pet’s immune response is expected to be adequate immediately after receiving the booster.
If exposure to a rabies-risk species has occurred, contact your veterinarian to arrange another rabies vaccine booster for your vaccinated pet. At-home observation for 45 days is indicated. Some unvaccinated animals will mount an effective enough immune response if given early post-exposure treatment. The pet would need a strict six-month quarantine after receiving the vaccine if the animal it was exposed to could not be tested or tested positive for rabies. If the veterinarian suspects rabies, the affected animal is humanely euthanized to prevent suffering.
Bat exclusion
Saskatchewan has a Bat Exclusion Policy that outlines requirements and procedures for capturing, handling, excluding, and removing bats from any buildings or structures. It is illegal to interfere with, harass, kill, or disturb bats and their roosting sites since they are protected wildlife. For this reason, a permit is required to exclude them from any building that they may have moved into. Additionally, exclusion is only permitted during certain months of the year. Here is a breakdown of bat-friendly exclusion timing:
| Bat exclusion is… | Month | Reason |
| Allowed | May | Bats are pregnant and would be able to find a new home if they are excluded from a building |
| Possible* | June – August | Bats are birthing their pups which cannot fly, mothers would be separated from their young who would be left to starve |
| Allowed | September | Bats are mating, pups are flying and moving to winter habitats |
| Possible* | October – April | Bats are mating, pups are flying and moving to winter habitats
Bats are hibernating |
*Bat exclusion is possible if certain conditions are met. Contact the Ministry of Environment for information.
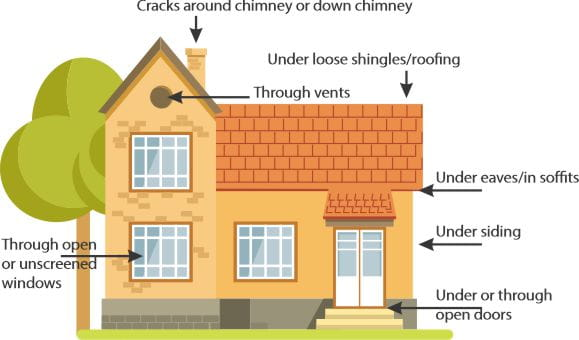
The bat exclusion process allows bats to leave a building safely and then seals the exterior access point to prevent them from reentering (Figure 3). If the risk of direct contact with the bats is low and people can still use the space safely, evicting bats from a building is not always necessary.
We are still unsure why we received more bat submissions in 2025 than in previous years. Is the population of bats in the urban environment increasing? Are there more bats suffering from their proximity to humans? Are people more aware of CWHC’s work and Public Health’s interest in testing bats and are submitting more bats for post-mortem exams? This is something yet to be understood, but this blog article can answer some of the common questions that people may have regarding bats in all of these possible contexts. We hope this article helps spread awareness on the importance of bats and which threats they face. If you have any other questions regarding this topic or anything related to Canadian wildlife, please don’t hesitate to leave a comment or contact us at **@*******sf.ca.
Written by Sabine Kirsch and Beatriz Garcia de Sousa, and revised by Trent Bollinger, Ursula Perdrizet, and Shelagh Copeland.
References
Bat Conservation International (2026, March 3). Bat Conservation International. https://www.batcon.org/
Bat Encounters. (n.d.). Government of Saskatchewan. Retrieved April 2, 2026, from https://www.saskatchewan.ca/residents/environment-public-health-and-safety/wildlife-issues/living-with-wildlife/bats-in-saskatchewan/bat-encounters
Rabies in Canada. (n.d.). Canadian Veterinary Medical Association. Retrieved April 2, 2026, from https://www.canadianveterinarians.net/about-cvma/latest-news/rabies-in-canada/
Rabies. (2025, December 18). HealthLink British Columbia. Retrieved April 2, 2026, from https://www.healthlinkbc.ca/healthlinkbc-files/rabies
Rabies vaccines: Canadian immunization guide. (2025, January). Government of Canada. Retrieved April 2, 2026, from https://www.canada.ca/en/public-health/services/publications/healthy-living/canadian-immunization-guide-part-4-active-vaccines/page-18-rabies-vaccine.html
Ramírez‐fráncel, L. A., García‐herrera, L. V., Losada‐prado, S., Reinoso‐flórez, G., Sánchez‐hernández, A., Estrada‐villegas, S., Lim, B. K., & Guevara, G. (2021). Bats and their vital ecosystem services: a global review. Integrative Zoology, 17(1), 2–23. https://doi.org/10.1111/1749-4877.12552
Segers, J., McBurney, S., Jones, M., Zimmer, P., Joly, D. (2024). The Canadian Wildlife Health Cooperative Annual National Bat Health Report – 2024. Retrieved April 9, 2026, from https://www.cwhc-rcsf.ca/docs/bat_health/CWHC%20National%20bat%20health%20report%20%20-%202024.pdf
Wilson, A. G., Fehlner-Gardiner, C., Wilson, S., Pierce, K. N., McGregor, G. F., González, C., & Luszcz, T. M. J. (2022). Assessing the extent and public health impact of bat predation by domestic animals using data from a rabies passive surveillance program. PLOS Global Public Health, 2(5), e0000357. https://doi.org/10.1371/journal.pgph.0000357

